Uncomfortable Sanity: Cortisol Addiction and the Brain
The effects of stress and cortisol addiction on one's ability to just freakin' vibe.
Therapy made me hear voices in my head.
Good news? They’re all mine.
Bad news? I’m constantly having a conversation with myself. Well, conversation is a bit euphemistic—it’s more like an argument.
The fight goes something like this:
Rae 1: I feel happy.
Rae 2: Well, that can’t be good. Something must inevitably fail. Shall we self-sabotage?
Rae 1: No, we don’t do that anymore.
Rae 2: Sure, but we’re really good at it.
Rae 1: We’re also really good at taking tequila shots, that doesn’t mean it’s good for us.
Rae 2: Right, but hear me out. We feel happy right now, and then what happens? We let our guard down. We get comfortable. BANG. Abandonment. Failure. Despair. But if we fuck up now, at least it’s on our terms. Thoughtsies?
Rae 1: You really fucking suck sometimes, you know that? This is why we can’t have nice things.
Rae 2: Fine, (mockingly) we can be happy. Play your little games, grow your little career, have your little hopes and dreams. But when it all comes crashing down, remember I warned you. I tried to keep you safe.
Now, Rae 2 is a total dick, but she can’t help it. She’s addicted to cortisol.
Much like any substance, if you provide your body with enough of something over a regular enough cadence, it starts to think it belongs there. Sometimes, this is good. This is how vaccines work: we put a little bit of sickness into the body, body goes “huh, that’s new,” body creates antibodies, antibodies become part of the body and the body is fine with this because it comes to expect them—they’re supposed to be there.
Cortisol is supposed to be there, but it is not supposed to be an all-day, everyday kind of thing. Cortisol is designed to serve two main purposes:
Helping you survive (hello fight or flight)
Waking you up (rude)
When you grow up or spend prolonged amounts of time in an unsafe or tumultuous environment, you’re constantly in a state of heightened awareness, so you’re constantly releasing cortisol. In theory, this is how it’s supposed to work—there is a threat to your safety, your brain responds to that.
But when you’re constantly living in a state of fight or flight, your brain starts to work backward. Since you’re always looking for that next hit, chaos and pain become what feel good, and safety and peace become the threats. Safety and peace don’t produce cortisol and, since we’re stress addicts now, safety and peace don’t feel good. Stress becomes your resting state—your body gets used to it and thinks it’s always supposed to be there, and you begin to actively seek out situations that can produce it. Stress is familiar, stress is home.
We are now stuck in a system where we can only feel good if we are on edge or unsafe, and we do irreversible damage in the process.
Cortisol and the Brain
Cortisol addiction and stress addiction can cause a variety of symptoms and side effects including:
Insomnia and Fatigue
Headaches
Digestive problems
Anxiety and Depression
Irritability and Mood swings
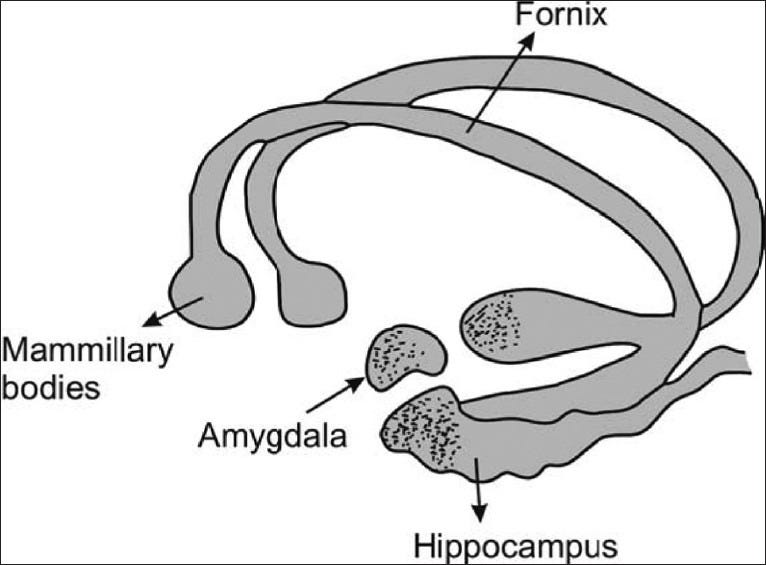
But the scariest side effect of all is cortisol's direct effect on the hippocampus. The hippocampus is a brain structure within the temporal lobe that plays a crucial part in learning and memory.
It’s about to get real nerdy up in here, so if you don’t want to geek out on the science, TLDR: an excess of cortisol impairs the brain’s ability to both form and recall memories by both damaging and decreasing the volume of the hippocampus and several other brain regions. Constant stress literally shrinks your brain.
This is your brain on drugs (cortisol)
Repeated cortisol exposure can cause inflammation all over the body and, over time, has the ability to break down the blood-brain barrier and allow these circulating inflammatory proteins to enter the brain and cause a variety of issues such as hippocampal shrinkage, mood disorders, and a decrease in motivation and mental agility.
In fact, cortisol and high-stress levels are so detrimental to the brain that rates of hippocampal atrophy—often caused by stress—are a key diagnostic and prognostic marker for Alzheimer’s disease. The worst part? The higher the rate of hippocampal atrophy, the less the brain is able to control cortisol release.
In complex terms, “the hippocampus inhibits the hypothalamo-pituitary-adrenal axis. When cortisol is elevated, it can induce hippocampal atrophy, which “lifts the brake” on the hypothalamo-pituitary-adrenal axis. The resulting cortisol increase induces further hippocampal atrophy, resulting in a vicious circle.”
In the simplest terms possible, cortisol damages the brain, the brain cannot control cortisol output, more cortisol is released.
Stress can also affect the accuracy of memories over time. Stress at the time of an event positively influences memory, but stress at the time of recollection impairs memory. When recalling the memory later, if stress is induced, the memory becomes susceptible to other influences, such as suggestions from other people, or emotions unrelated to the event but present during recall.
This means that over time, stress has the ability to taint positive memories. You see this effect in people who struggle with PTSD and depression (both also linked to repeated stress exposure). They can’t remember when things were good, or they can’t feel that they’ve experienced joy, wonder, hope, etc. The effect of repeated stress and cortisol exposure has superimposed present-day emotions on past memories.
Not only does stress inhibit your ability to recall memories and learn, stress also affects the area of your brain known as the prefrontal cortex which is key in decision-making. From an evolutionary standpoint, this makes sense. If a bear is running towards you, you don’t really have time to sit down and make thoughtful, informed decisions. You have to react impulsively; run or fight the bear (disclaimer: I do not recommend fighting bears).
However, day-to-day operations require forethought and intention. You can’t be treating every interaction as a life-or-death threat, but this is the reality for cortisol-addicted people. Every situation is a dangerous one and every person you interact with is a potential enemy. Stress impairs your ability to properly assess scenarios, understand intentions, and assign trust. All of these are key factors in building and maintaining healthy relationships.
Me and My Gang of Traumatized Homies™
Birds of a feather flock together, which means I am blessed to be surrounded by people who are fighting the same fight I am. Life was hard, childhood was brutal. We couldn’t do much about it as kids, so we’re trying to clean it up and get it together as adults.
Being surrounded by people who have also experienced trauma and adversity that has been mentally and chemically altering leads to some wonderful and difficult conversations. Most recently, the theme has revolved around the inability to find solace in safety and interpersonal relationships. So many of my friends and loved ones view intimacy and intention as a threat.
They can understand when a man wants to hit them, but not when he wants to hold them. They can understand when a boss provides criticism, but not when she provides praise. They can tolerate loneliness better than being surrounded by people who love them. The association has become that human connection is innately painful. Pain makes sense, comfort doesn’t.
We ask each other questions like:
“How do you handle the transition from anxious attachment to now being severely avoidant?”
“Are you able to tolerate when he’s actually nice and present, or does that trigger your anxiety?”
“What about that relationship made you tolerate the abuse? What about your past made you think you deserved it?”
In our own, messed-up kind of way, we’re navigating our brain damage together. Sometimes, we simply laugh at how ridiculous it all is. Someone will say something like, “he texted me back right away, and it gave me the ick,” or “yea, I like her a lot. I think I’m going to ghost her,” and you can’t help but smile. The second the words leave your mouth, you realize how fucked up it all sounds. But that recognition is evidence of healing, and sometimes that’s enough.
We frequently have to force ourselves to sit in safety in the same way other people have to force themselves to sit in discomfort. At times, our comfort in discomfort has been beneficial. We have no problem diving headfirst into things other people would find paralyzing because they are uncomfortable; moving across the country, changing careers, doing things by ourselves, and living impulsively for the plot to see where it takes us. However, we find ourselves struggling with things other people find easy: opening up, relaxing, doing things with intention, and accepting help.
The most interesting part of healing is that the “old you” still exists. It needs to be spoken to, reassured. Sometimes, it needs to be fought with. Most times, it needs to know it’s not alone. Because you’re not alone.
I wish I’d known years ago the things I know today, but I didn’t. I wish I had the friends I have today who tell me, “you’re not crazy, I feel this way too,” but I didn’t. I wish mental health had been a bigger conversation for our parents’ generation so that it didn’t fall on ours to pick up the pieces, but it wasn’t. I wish we all had grown up in homes that felt loving, safe, and nurturing so that we could accept love and intimacy and life didn’t feel like an uphill battle. But we didn’t.
We are doing the best we can with what we’ve been given and that’s all we can do.
Keep healing. Keep laughing at your trauma. Keep talking to your friends. Keep fighting yourself.
After all, even if the voice in your head is right and it all does fall apart, it’s nothing we haven’t survived before. We can do it again.
Here’s to you, to me, and to our brains—a little bit damaged, but built to survive.